About
TGCT
What is tenosynovial giant cell tumor (TGCT)?
TGCT, formerly known as pigmented villonodular synovitis (PVNS), is a rare disease where non-malignant (benign) tumors form in the joint, causing pain, stiffness, and loss of function. Over time, these changes can permanently affect the joint and nearby tissues.
There are only 11-50 cases of TGCT per million people each year.
92
%
of people with TGCT
experienced pain*
85
%
of people living with
TGCT
reported swelling*
*According to a survey of 497 patients with TGCT
LIVING WITH TGCT
TGCT is so much more than pain alone. For many, it affects how they move, how they feel, and how they live day-to-day. Even though TGCT is considered non-life threatening, it can still weigh on everyday activities and overall well-being.
Physical Impact
Pain is the most common symptom. Swelling, stiffness, and reduced range of motion in the joint are also reported.
said pain interfered with overall enjoyment of life*
Emotional & Financial Impact
Patients often describe feeling frustrated, anxious, and isolated due to delayed diagnosis, tumor recurrence, or being misunderstood.
In a separate survey,
with rare diseases reported experiencing anxiety and stress compared to 17% of the general population
A TGCT diagnosis can significantly increase medical and physical therapy costs.
Impact on
Daily Life
reported that pain interfered with their day-to-day activities*
TGCT pain can make daily life harder, especially social activities, chores, and family life. Tasks like concentrating, walking, and running errands may also become difficult.
changed jobs or retired early because of TGCT*
*According to a survey of 497 patients with TGCT
What causes TGCT?
Research shows that TGCT forms when cells make too much of a protein called colony-stimulating factor 1 (CSF1), which causes tumor growth. This protein attracts immune cells expressing colony stimulating factor 1 receptor (CSF1R), leading to inflammation and swelling. TGCT can lead to potentially permanent joint damage in some cases.
PVNS? GCT‑TS?
It’s all TGCT
TGCT used to be referred to as pigmented villonodular synovitis (PVNS) and giant cell tumor of the tendon sheath (GCT-TS). In 2013, the World Health Organization reclassified GCT-TS, PVNS and diffuse-type giant cell tumor all as TGCT.
The various names can be confusing, but when in doubt, just remember PVNS and GCT-TS are all the same disease: TGCT.
SEE GLOSSARY OF TERMS
2 TYPES of TGCT
There are two types of TGCT: localized/nodular and diffuse. Localized/nodular TGCT tends to be smaller tumors inside of the joint, while diffuse TGCT tumors are larger, without distinct boundaries.
Your experience may be different from other patients depending on your type of TGCT and tumor location.
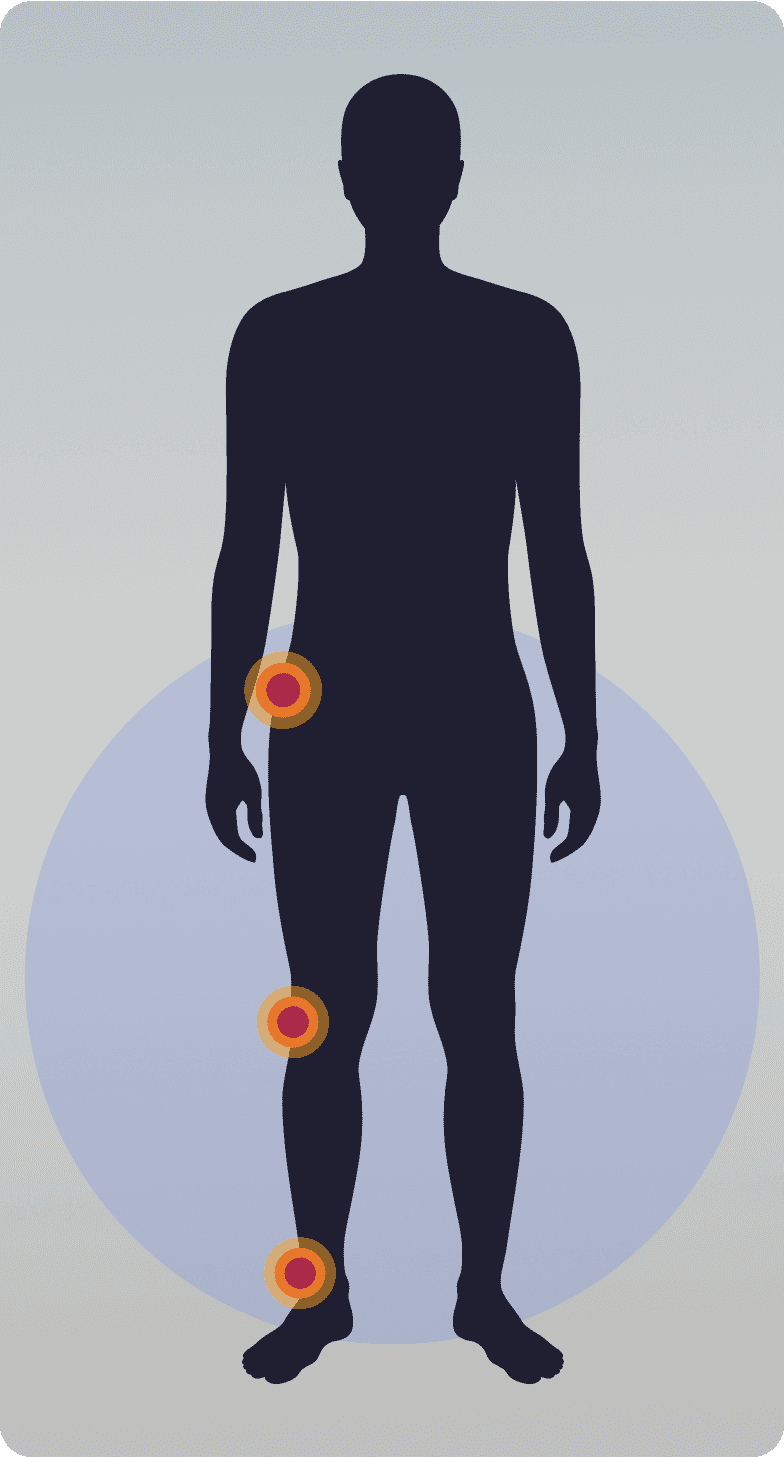
Localized/
nodular TGCT
More common
Lifetime recurrence rate: up to 15%
Usually single, well-defined tumor, usually nodular
Often does not cause pain or joint dysfunction
Tumor location:Tends to impact smaller joints like hands, fingers, wrist, feet
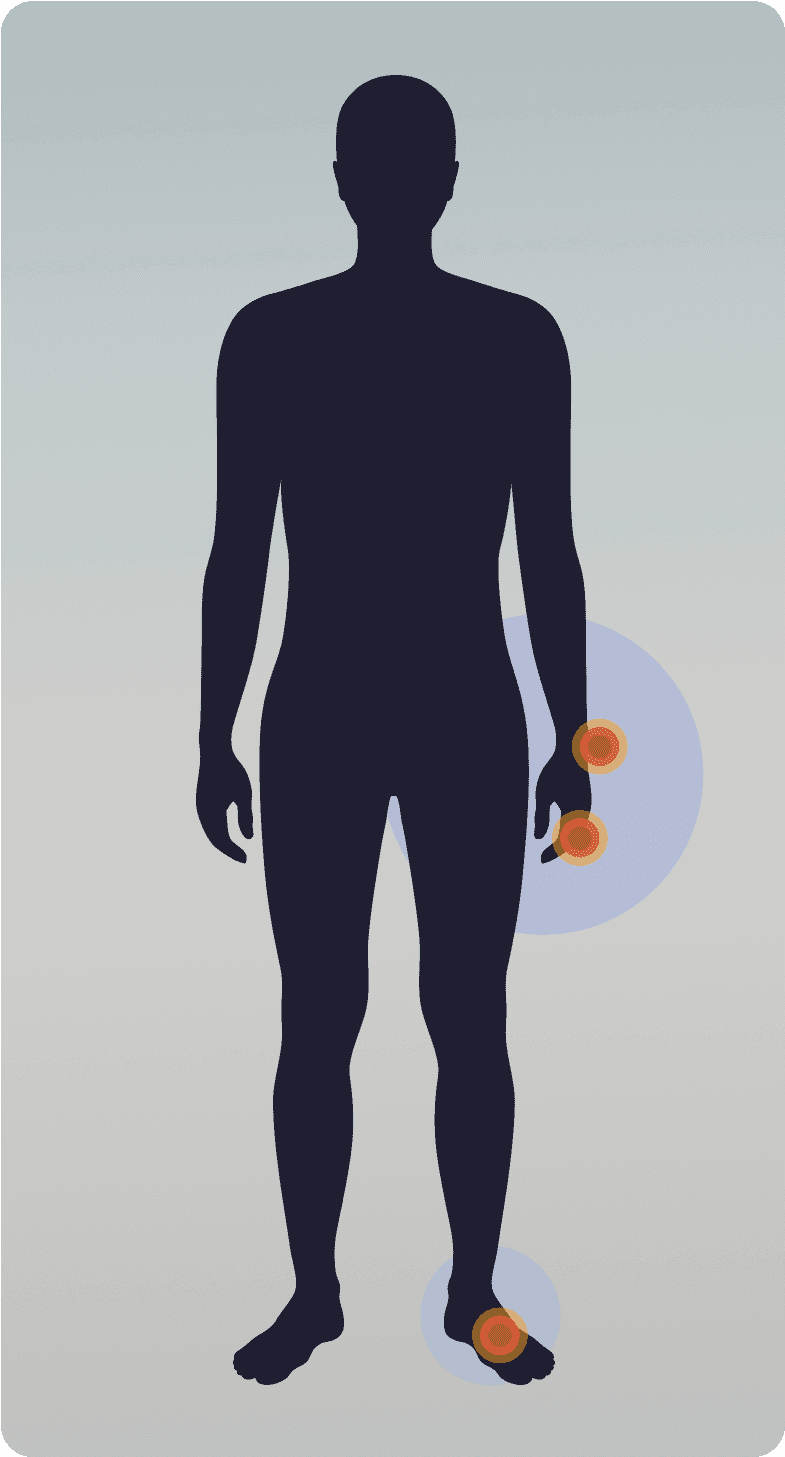
Diffuse TGCT
Less common
Lifetime recurrence rate: up to 72%
lll-defined tumors that invade the joint
Can extend out of the joint and damage surrounding bone
Tumor location:Tends to impact larger joints like knee, hip, ankle
In a survey of 289 people
living with TGCT,
72
%
of people with diffuse TGCT had
at least 1 recurrence after surgery
Signs & Symptoms
Patients with symptomatic TGCT often suffer from:
Pain
Swelling
Stiffness
Instability
Reduced range of motion
Diagnosing TGCT
Getting diagnosed with TGCT can be a journey in itself. Symptoms can mimic those of other diseases and not all doctors have experience with TGCT, which is why it's crucial to consult an oncologist or doctor who treats TGCT.
FIND A TGCT SPECIALISTTGCT Support is an independent organization that is not affiliated with Deciphera. Deciphera is not responsible for the content on TGCT Support's website or any services or materials it may provide, including development of and/or information contained in the TGCT Specialist List (the “List”). This link is being provided for informational purposes only. Deciphera does not endorse or recommend any specific physician or center included in the List and makes no representations or warranties about the services they provide.
IT CAN TAKE UP TO
3-4 YEARS
TO GET A TGCT DIAGNOSIS
There are multiple steps to a TGCT diagnosis, which can include the following:
Physical exam
Full analysis of medical history
X-ray
MRI
CT scan
Biopsy
While there are various options for imaging, an MRI is recommended, followed by a biopsy. A definitive diagnosis of TGCT is normally obtained through a biopsy and will help you and your care team understand what treatment option may be best for your specific TGCT.
Greater awareness may help people get diagnosed earlier and access treatments sooner.
CT=computed tomography;
MRI=magnetic resonance imaging.